
Firefighters battle the Woolsey Fire Nov. 11 in Malibu, Calif. (CNS photo/Reuters/Eric Thayer)
For several days in August, a grey pall of smoke and ash settled over Seattle and the surrounding Puget Sound region.
The smoky haze that blanketed the skies of the Pacific Northwest metropolis came from all sides: wildfires to the south in Oregon and northern California, wildfires to the east beyond the Cascades, wildfires to the north in Canada's British Columbia.

The well-traveled smoke plummeted air quality in Seattle and also led to an upsurge in trips to the Providence St. Joseph emergency room.
"There was just ash raining down like snow at some points," said Richard Beam, the Catholic hospital system's chief environmental officer, who lives on Bainbridge Island across the Sound from Seattle. "And so we were having an increase of people coming to us with asthma and other lung-associated illnesses. Breathing, having a difficult time breathing."
More and more, Catholic and other health care providers are recognizing how the effects of climate change, such as stronger and more destructive wildfires, are harming human health and will only worsen as the planet warms.
But as the medical community examines its response to climate change, a discomfiting realization has become apparent: They're part of the problem.
While hospitals play a pivotal role in treating patients and communities dealing with health issues developing from the fallout of rising temperatures, they also represent one of the largest sources of the air pollutants warming the planet.
A 2016 study found the U.S. health care industry as a whole accounts for roughly 10 percent of the nation's total greenhouse gas emissions. It is also the seventh-largest carbon emitter globally. A separate 2016 analysis from the U.S. Energy Information Administration found hospitals behind only the food service industry in terms of energy consumption from buildings.
It's a contradiction the health care world is becoming more aware of and increasingly intent on addressing.
"Health care has a mission to first do no harm. And here we have a sector that nevertheless has a tremendous carbon footprint, that is contributing to climate change and also to air pollution," said Sarah Spengeman, an associate director of the U.S. climate and health program for Health Care Without Harm, a nongovernmental organization that works with hospitals worldwide to implement sustainable and environmentally friendly initiatives.
A bedrock issue
Though the wildfires in some cases burned hundreds of miles away from the Puget Sound, the intensity was so great that the lingering, sun-blotting smoke that drifted to Seattle dropped the city's air quality to unhealthy levels — the equivalent of smoking seven cigarettes a day— and to worse than in Beijing, the Chinese capital with the ignominious title as home to some of the worst smog and air pollution in the world.
Wildfire smoke can cause coughing, stinging eyes, headaches, irritated sinuses and shortness of breath. In more severe cases, the particulates it puts into the air can exacerbate the risk of asthma attacks along with numerous pulmonary and cardiovascular issues, including heart attacks, pulmonary embolisms and strokes.
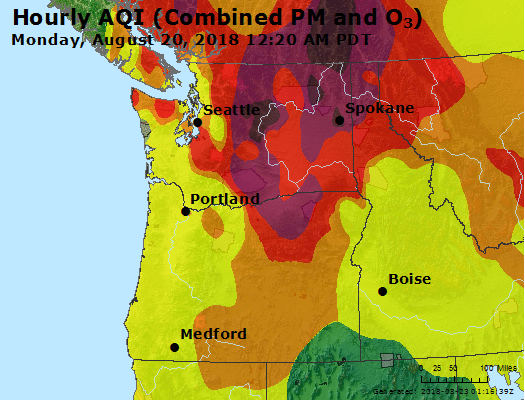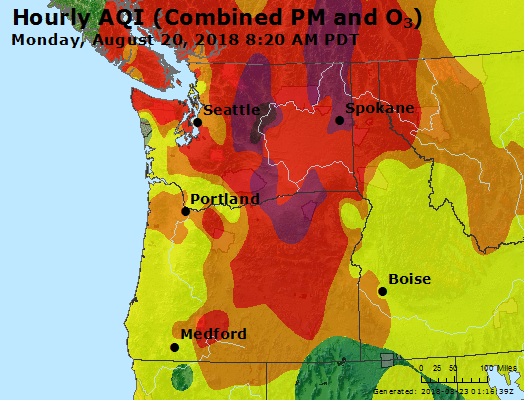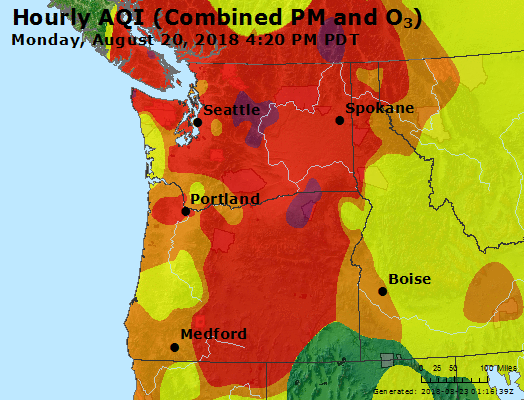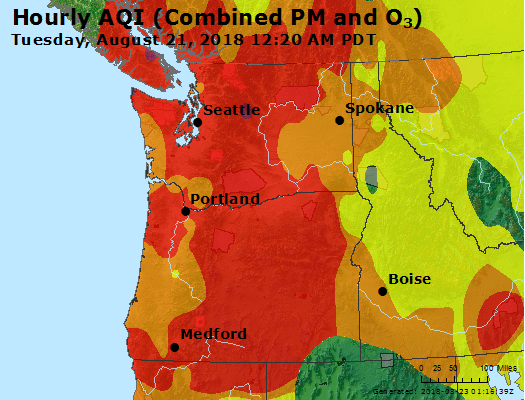
"Wildfires are creating a public health crisis that is growing in severity as the number, size and frequency of wildfires increase," wrote Lloyd Dean, president and CEO of Dignity Health, in an August op-ed for the journal Health Affairs. "For me, this is yet another indication that the health of our environment is closely linked to the health of our communities."
Groups like Health Care Without Harm and Catholic Health Association have worked to educate its member hospitals on the relationship between climate change and health, and to encourage them to take steps to minimize their own carbon footprints.
For Catholic hospitals, such action stems from their moral tradition, said Julie Trocchio, CHA senior director for community benefit and continuing care, and a recognition that climate impacts are often most felt by the poor and vulnerable communities — a population already prominent on the radar of health care providers.
"When we say it's a moral issue, we're particularly concerned about the poor," she told NCR. "And that is certainly one of the bedrock issues for Catholic health care, a special concern for vulnerable people."
"Health care has a mission to first do no harm. And here we have a sector ... that is contributing to climate change and also to air pollution."
—Sarah Spengeman
The U.S. government's Fourth National Climate Assessment dedicates two chapters to climate change and health and its impact on air quality. The report, compiled by 13 federal agencies and released in November, is succinct in its conclusion on the connection between the climate and health:
"The health and well-being of Americans are already affected by climate change, with the adverse health consequences projected to worsen with additional climate change. Climate change affects human health by altering exposures to heat waves, floods, droughts, and other extreme events; vector-, food- and waterborne infectious diseases; changes in the quality and safety of air, food, and water; and stresses to mental health and well-being."
Heat and health risks
Some of the effects are easy to connect. Hotter temperatures leading to more frequent and intense heat waves, for instance, are projected to lead to higher rates of heat-related illnesses, such as cardiovascular and respiratory complications, renal failure, preterm birth and negative effects on fetal health. Those most at risk are older adults, children and pregnant women.
The national climate report projected that extreme heat and cold will result in more than 9,000 additional premature deaths annually by the end of the century, with half avoidable by dramatically reducing emissions.
Other effects are less obvious.

A satellite image shows the wildfire Aug. 6 at the Mendocino Complex in California. The wildfires in California contributed to heavy smoke in southern Oregon, causing some parishes to move activities indoors and preventing some people from traveling to Mass. (CNS photo/DigitalGlobe, a Maxar company, handout via Reuters)
Warmer temperatures expand the geographic range of vector-borne diseases, like Zika and West Nile viruses, and prolong the lifespan of their carriers. According to the Centers for Disease Control, the number of reported cases of disease from mosquito, tick and flea bites has more than tripled from 2004 to 2016, and specifically tick-borne diseases more than doubled, with 82% being cases of Lyme disease. The U.S. climate assessment projects national cases of West Nile to double by 2050 as temperatures increase, and to produce an additional 3,300 cases, at a cost of $3.3 billion, by the end of the century.
As the planet warms, it's projected that harmful algae blooms, like the "red tide" in Florida that triggered a state of emergency declaration last summer, could linger in recreational waters a full month longer, producing toxins that can cause gastrointestinal illnesses and neurological disorders.
In addition, the trauma of losing a home or being displaced by a weather-related disaster — or for emergency workers, in responding to it — can bring about mental health issues.
"People who lose their homes due to an extreme weather event can suffer from PTSD or struggle with depression, maybe for the rest of their lives," Spengeman said. She added that a study from Stanford University published last year showed a correlation between periods of extreme heat and increased suicides.
In terms of health, the national climate report estimated reducing greenhouse gas emissions could yield "economic benefits of hundreds of billions of dollars each year by the end of the century," and that a low-emissions trajectory could halve the health impacts and associated costs compared to a high-emissions scenario.
Advertisement
That buoys a report from the United Nations' climate science body that keeping temperature rise below 1.5 degrees Celsius (2.7 degrees Fahrenheit) would prevent the exposure of 420 million people to severe heatwaves, and lower the risks of heat-related illness and death and the spread of vector-borne diseases. At present, the World Health Organization estimates between 2030 and 2050 that climate change will cause an additional 250,000 additional deaths per year, due to malnutrition, malaria, diarrhea and heat stress.
A major report from 250 scientists issued at the Fourth U.N. Environment Assembly in March stated "air pollution is the largest environmental health risk" and without changes to address rising emissions, it will lead to an estimated 4.5 million to 7 million premature deaths by midcentury.
Prodigious producers of waste
The U.S. climate assessment also projected that the nation's hospitals could see savings of $15 billion over the next decade by implementing basic energy efficiency and waste-reduction measures.
When Beam joined then-Providence Health in 1995 as a corporate energy manager, he said it was often cost that drove decisions about energy management, largely in terms of efficiency. "If we used less energy, we could save money."
Richard Beam, chief environmental officer of Providence St. Joseph Health (Courtesy of Providence St. Joseph Health)
While financial savings remain a prominent motivator, the past two decades have witnessed more recognition — a "tremendous shift" in perspective, as Beam called it — of the negative environmental impacts a hospital has on the community it strives to heal and serve.
"We realize it doesn't do anybody a lot of good to have them come into our health system to heal them in some way, only to put them back into an environment that's just going to continue to bring these kind of things back around again," he said.
"We know that we have these negative impacts on the health of people within the community by what we generate and through our operations," Beam added. "So we have a very clear obligation to help people improve their health through enhancing the environment that they're living in."
Beam describes hospitals as "prodigious producers of waste," at least from a resources perspective: Each is essentially a small city in itself that operates (i.e., uses electricity) 24 hours a day, puts a strain on water and sewer systems, and accumulates a daily tide of new supplies while simultaneously producing a myriad of waste streams, from medical to biological to general. All of those factors can impact community health, whether directly or indirectly.
As a Catholic health system, the moral dimension was always in mind but became more pronounced with the June 2015 publication of Pope Francis' encyclical "Laudato Si', on Care for Our Common Home." Beam said the document has had "a tremendous impact on Catholic health care," and has sparked them to strive to be "a world-class steward" of the earth.
Trocchio added the encyclical provided "additional spirit and motivation" for Catholic hospitals, many already taking steps on climate change.
"I think many hospitals were on the way, had realized how important climate change was and energy use was, but Laudato Si'really did propel it even more," she said.
Groups like Health Care Without Harm and Catholic Climate Covenant have been integral in providing resources and connecting health systems to each other and to the moral and scientific rationale for addressing climate change, along with keeping them apprised of what is happening industry-wise with environmental sustainability.

Julie Trocchio, senior director of community benefit and continuing care at Catholic Health Association (Courtesy of Catholic Health Association)
Another network, We Are Still In, emerged in the days after President Donald Trump announced he would withdraw the U.S. from the Paris Agreement on climate change. The coalition counts more than 2,700 partners composing states, cities, businesses, universities and faith groups, and health organizations — of the 28 signed on, six are Catholic; another 11 Catholic health care institutions joined through the Catholic Climate Declaration.
"We have that call from our moral tradition as well to look at how can we reduce our carbon footprint. And we've got lots of potential there because of our high energy use," Trocchio said.
"We come from a faith-based tradition," said Dominican Sr. Mary Ellen Leciejewski, vice president of corporate responsibility with Dignity Health. "And we realize that, you know, this is the planet we have. It's a gift. And so what is it that we can do to steward our resources to just show that it is a gift that we have, and we don't want to take it for granted?"
Keeping the drum beat going
Dignity Health, the fifth-largest health system in the country, was among the first health care systems to join We Are Still In. It has set across-the-board goals for reducing its carbon footprint by 2020:
- Cut its greenhouse gas emissions by 40% compared to 2010 levels (31% reduction, as of 2016);
- Decrease energy use by 20% (16% decrease as of 2016);
- Increase its renewable energy to 35% (13% as of 2016, including 27% of electricity);
- Decrease water use by 20% (2% reduction as of 2016);
- Decrease landfill waste by 40% (34% diversion rate).
Its 2018 sustainability report documented progress to date and the steps to get there across its nearly 40 acute care hospitals, located in California, Arizona and Nevada. In May, it brought online 2-megawatt and 1.7-megawatt solar plants at two of its Nevada hospitals. The system has also installed more than 150 charging stations for electric vehicles, replaced fluorescent lamps with LED versions in all its hospitals and eliminated plastic straws and drink stirrers from all its facilities.

In June 2018, the San Martin campus of Dignity Health-St. Rose Dominican Hospital, in Las Vegas, Nevada, brought online a 2-megawatt solar array. The nearly 6,000 solar modules, combined with a 1.7-megawatt solar array at its Sienna campus in Henderson, is expected to offset the environmental impact of roughly 1,000 cars each year. (Dignity Health)
Providence St. Joseph, also part of We Are Still In, has its own set of goals for its 51 hospitals and 829 clinics across seven states, including reducing its carbon footprint by 30% by 2025, and in the same time reducing its waste by half. It hopes to be carbon-neutral — removing as much carbon dioxide from the atmosphere as it produces — by mid-century.
As they work toward those goals, the West Coast-based systems also continue to measure how climate change is impacting its patients. Community health needs assessments, or CHNAs, allow health care professionals to track what ailments patients experience and how they change over time. With last year's wildfires, there was an uptick in asthma cases and other respiratory illnesses.
The toll of the fires struck close personally for some of Providence St. Joseph's health providers, whose homes burned while they cared for their patients. Dignity reported that 74 of its caregivers lost their homes to the Carr fire that burned through northern California and approached its medical center in Redding.
The extensive wildfires of recent years have made officials at Dignity Health more cognizant of the chemicals within different products they purchase, such as flame retardants in furniture, that put people and first responders further at risk. They have advocated for the removal of such unsafe chemicals.
They have also joined other health care systems on other advocacy fronts, including support for the Paris Agreement and opposition to the Trump administration's rollback of environmental regulations, most recently its effort to loosen rules on mercury emissions from power plants — more often located near low-income communities — that were estimated to prevent 11,000 premature deaths and 100,000-plus asthma attacks each year.
As the fires burned through the West last summer, and the smoke traveled throughout the country, Dignity Health and Providence St. Joseph joined with two other California health systems to form the California Health Care Climate Alliance. Together, they hope to redouble the health care sector's work in protecting the public from climate impacts, while also aiding the state in achieving its climate targets: becoming carbon neutral and removing carbon from its electricity grid by 2045.
Early this year, Dignity Health released its own 2025 goals. Leciejewski said that they and other hospital systems are on a mission to live out their mission by addressing the health threats brought by climate change, while also curbing their own contributions to the problem.
"Keep that drumbeat going that we're here and we want to do this together," she said. "And it is for the health and the safety of everyone."
[Brian Roewe is an NCR staff writer. His email address is [email protected]. Follow him on Twitter: @BrianRoewe.]







